NEW YORK, HERTFORDSHIRE, England and PITTSBURGH – April 18, 2019 – Non-profit drug developer, TB Alliance, and pharmaceutical company, Mylan N.V. (NASDAQ: MYL), today announced a global collaboration to make the experimental drug pretomanid accessible for use in two investigational drug regimens for pulmonary tuberculosis (TB).
TB, a bacterial infection transmitted through the air, is a challenging disease to treat, often requiring treatment through a combination of antibiotics. It also is the leading cause of death among people with HIV/AIDS1 and accounts for more than 1 in 4 fatalities from antimicrobial resistance annually.2 TB occurs in every part of the world. In 2017, the largest number of new TB cases occurred in the Southeast Asia and Western Pacific regions, followed by the African region. There is a growing resistance to available drugs, which means the disease is becoming deadlier and more difficult to treat. There were 558,000 cases of drug resistant TB in 2017.1
Multidrug resistant- (MDR) and extensively drug resistant- (XDR) TB are forms of the disease caused by bacteria that do not respond to first-line anti-TB drugs. Current treatments, therefore, consist of combinations of many different drugs, which may need to be taken for up to two years. Patients may take as many as 20 pills a day, resulting in numerous side-effects and often creating a significant economic burden.3 Drug sensitive- (DS) TB treatment, which consists of treatment with up to four drugs daily for six to nine months, has traditionally fared better with a global treatment success rate of approximately 82%; however, rising rates of resistance are complicating treatment and necessitating different options.1
“The TB drug pipeline is showing significant promise as we progress in our goal to provide transformative benefit to people with TB,” said Mel Spigelman, President and CEO of TB Alliance. “We are determined to take steps now to ensure that pretomanid, if approved, will be able to reach patients in need as part of an appropriate treatment regimen.”
Mylan CEO Heather Bresch added, “For more than a decade, Mylan has led the charge in accelerating access to high quality and affordable antiretrovirals for people living with HIV all over the world. We look forward to collaborating with TB Alliance to bring that same level of commitment and innovation to the millions of people suffering from tuberculosis, many of whom also have HIV. The drug regimens under development represent an important step in transforming the TB treatment landscape.”
Advancing Treatment for Patients
Pretomanid is a new chemical entity and a member of a class of compounds known as nitroimidazooxazines. TB Alliance began preclinical development of pretomanid in 2002, and it has since studied pretomanid in 20 clinical trials alone or in combination with other anti-TB drugs. Pretomanid has been administered in a clinical trial setting to more than 1,200 people in 14 countries.
The two pretomanid-based regimens under development include:
- For XDR-TB and MDR-TB that is treatment-intolerant or non-responsive: All oral, six to nine month treatment regimen consisting of bedaquiline, pretomanid and linezolid (“BPaL” regimen)
- For DS-TB and MDR-TB: All oral, four and six month treatments, respectively, consisting of bedaquiline, pretomanid, moxifloxacin and pyrazinamide (“BPaMZ” regimen)
TB Alliance is currently advancing the development of pretomanid in three ongoing late-stage clinical trials. The Nix-TB and ZeNix trials are evaluating the BPaL regimen for treatment of XDR-TB and related highly resistant forms of TB, while the SimpliciTB trial is evaluating the BPaMZ regimen for the treatment of DS-TB in four months and MDR-TB in six months.
The BPaL regimen has been studied in the ongoing Phase 3 Nix-TB trial, an open-label, single arm trial. Nix-TB participants with XDR-TB and treatment-intolerant or non-responsive MDR-TB were treated with bedaquiline, pretomanid and linezolid over six months, extended to nine months in some cases, with the intent to cure. In interim results from the first 75 participants presented at the 2018 Union World Conference on Lung Health, 89% of the trial participants had a favorable outcome with their clinical infection resolved and sputum cultures negative for TB after six months of treatment and six months of post-treatment follow-up.4
The BPaMZ regimen is being studied in the ongoing late-stage SimpliciTB clinical trial, initiated in 2018, for the treatment of both DS- and MDR-TB. The BPaMZ regimen was previously evaluated in TB Alliance’s Phase 2b study called NC-005, in which people with MDR-TB who were treated with the BPaMZ regimen cleared TB bacteria from their lungs up to three times faster than drug-sensitive TB patients treated with the standard first-line treatment (HRZE).5
A Global Commitment
The collaboration between Mylan and TB Alliance includes a global license from TB Alliance to Mylan for pretomanid for use in the following regimens:
- As part of the BPaL regimen, TB Alliance has granted a license to Mylan to manufacture and commercialize pretomanid, pending regulatory approval, for XDR-TB and treatment-intolerant or non-responsive MDR-TB. The BPaL regimen includes bedaquiline, which is exclusively manufactured and marketed by the Janssen Pharmaceutical Companies of Johnson & Johnson (Janssen) outside of DS-TB, and linezolid, which is available from multiple manufacturers, including Mylan. A New Drug Application for pretomanid as part of the BPaL regimen is currently under Priority Review by the U.S. Food and Drug Administration.6 In addition, a marketing authorization application for pretomanid as part of the BPaL regimen is under review by the European Medicines Agency. Janssen will retain the exclusive rights to market bedaquiline including as part of any combination therapy for the treatment of MDR-TB for the term of its patents.
- As part of the BPaMZ regimen, TB Alliance has licensed pretomanid to Mylan for DS- and MDR-TB, and has granted a sublicense for bedaquiline to Mylan, for its development and commercialization for use in DS-TB only, under its license agreement with Janssen Pharmaceutica N.V., one of the Janssen Pharmaceutical Companies of Johnson & Johnson. Janssen has granted its consent to this sublicense. If the BPaMZ regimen is proven successful in the SimpliciTB trial, Mylan will seek regulatory approval of pretomanid as part of the BPaMZ regimen in DS-TB and MDR-TB as well as bedaquiline as part of the regimen in DS-TB. As with the BPaL regimen, Janssen will retain the exclusive rights to market bedaquiline as part of the combination therapy for the treatment of MDR-TB for the term of its patents.
Under the terms of the agreements comprising the collaboration and pending regulatory approvals, Mylan anticipates being the first company with the license to commercialize pretomanid for use in these regimens in certain low- and middle-income countries, where the vast majority of the global TB burden is located. The license agreement for pretomanid for the aforementioned countries will be non-exclusive, reflecting the commitment by TB Alliance and Mylan to ensure affordable and sustainable access to new TB treatments from multiple sources. Mylan has an exclusive license agreement for commercializing pretomanid for use in the BPaL and BPaMZ regimens in high-income markets.
Moving forward, TB Alliance and Mylan will work together to support antimicrobial stewardship and ensure that upon introduction, pretomanid is accessible to those who need it in the appropriate treatment regimen, pending regulatory approval and the issuance of new treatment guidelines by the World Health Organization.
About TB Alliance
TB Alliance is a not-for-profit organization dedicated to finding faster-acting and affordable drug regimens to fight TB. Through innovative science and with partners around the globe, we aim to ensure equitable access to faster, better TB cures that will advance global health and prosperity. TB Alliance operates with support from Australia’s Department of Foreign Affairs and Trade, Bill & Melinda Gates Foundation, Germany’s Federal Ministry of Education and Research through KfW, Global Health Innovative Technology Fund, Indonesia Health Fund, Irish Aid, Medical Research Council (United Kingdom), National Institute of Allergy and Infectious Disease, Netherlands Ministry of Foreign Affairs, United Kingdom Department for International Development, UK Department of Health, and the United States Agency for International Development.
About Mylan
Mylan is a global pharmaceutical company committed to setting new standards in healthcare. Working together around the world to provide 7 billion people access to high quality medicine, we innovate to satisfy unmet needs; make reliability and service excellence a habit; do what's right, not what's easy; and impact the future through passionate global leadership. We offer a growing portfolio of more than 7,500 marketed products around the world, including antiretroviral therapies on which more than 40% of people being treated for HIV/AIDS globally depend. We market our products in more than 165 countries and territories. We are one of the world's largest producers of active pharmaceutical ingredients. Every member of our approximately 35,000-strong workforce is dedicated to creating better health for a better world, one person at a time. Learn more at Mylan.com. We routinely post information that may be important to investors on our website at investor.mylan.com.
To read this announcement at Mylan's website, please click here.
Contacts
Mylan:
Christine Waller (Media)
724.514.1968
Email: communications@mylan.com
Melissa Trombetta (Investors)
724.514.1813
Email: InvestorRelations@mylan.com
TB Alliance:
Thomas Lynch
646.616.8639
Email: communications@tballiance.org
1. UNAIDS: http://www.unaids.org/en/topic/tuberculosis
2. Review on Antimicrobial Resistance: https://amr-review.org/
3. MSF: https://www.msf.org/tuberculosis
4. The 49th Union World Conference on Lung Health: https://thehague.worldlunghealth.org/2018/10/encouraging-drug-resistant-tb-treatment-results/
5. Conference on Retroactive and Opportunistic Infections, 2017: http://www.croiconference.org/sessions/efficacy-bedaquiline-pretomanid-moxifloxacin-pza-bpamz-against-ds-mdr-tb
6. TB Alliance: https://www.tballiance.org/news/pretomanid-enters-FDA-review
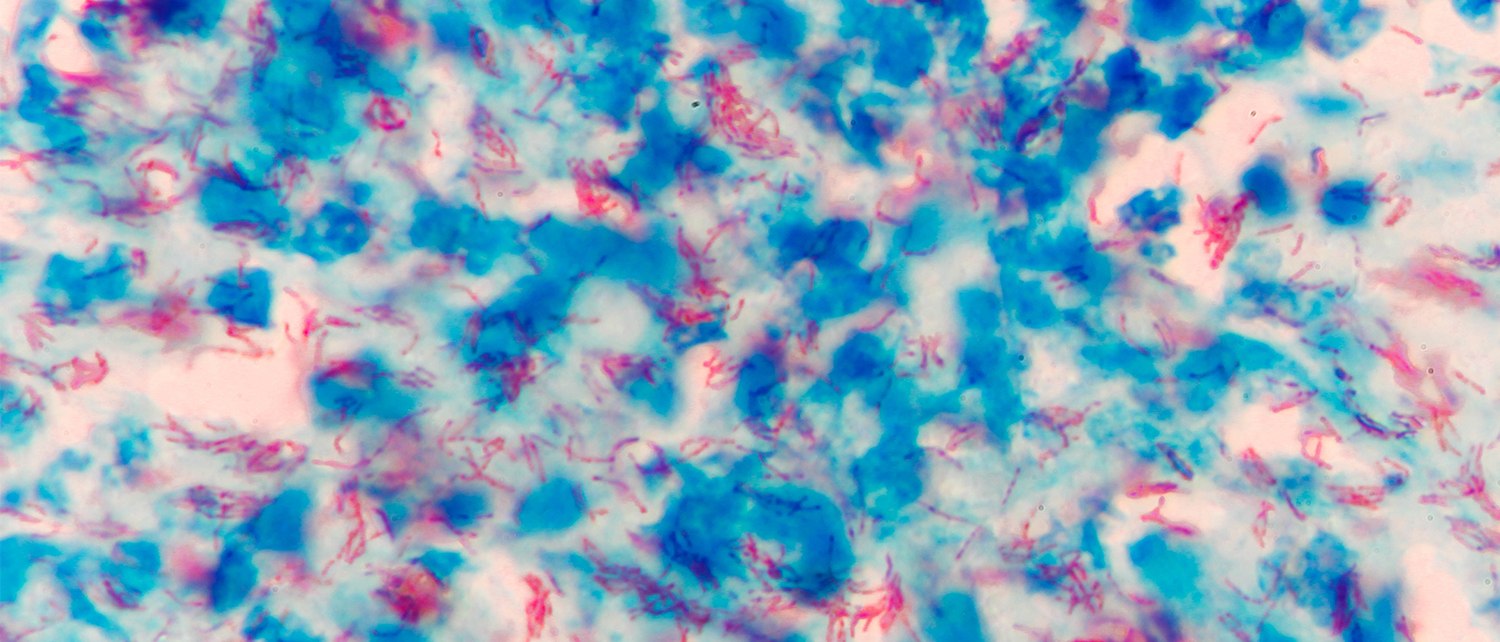
Photo caption: Microscopic view of mycobacterium tuberculosis – the bacteria that causes TB